Intended for healthcare professionals
Antipsychotic use in people with dementia

Assessment of diplopia in adults
Double vision, or diplopia, may be the first sign of sight or life threatening pathology. How should clinicians examine a patient with diplopia?
Assessment of diplopia in adults
Double vision, or diplopia, may be the first sign of sight or life threatening pathology. How should clinicians examine a patient with diplopia?


Argentina’s healthcare is crumbling under its worst ever dengue epidemic and Milei’s presidency
Argentina’s healthcare system is under threat. Martín de Ambrosio reports
Argentina’s healthcare is crumbling under its worst ever dengue epidemic and Milei’s presidency
Argentina’s healthcare system is under threat. Martín de Ambrosio reports

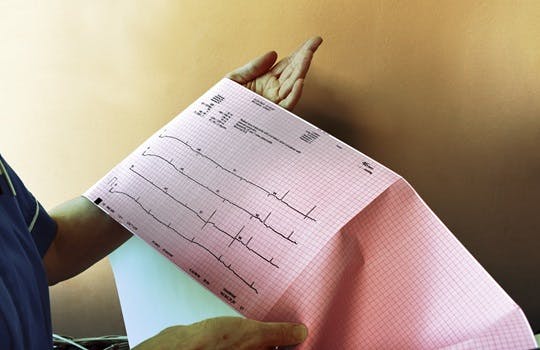
Temporal trends in lifetime risks of atrial fibrillation and its complications
The lifetime risk of atrial fibrillation has increased from one in four to one in three over the past two decades, finds this study
Temporal trends in lifetime risks of atrial fibrillation and its complications
The lifetime risk of atrial fibrillation has increased from one in four to one in three over the past two decades, finds this study

Losing NHS doctors early is costing £2.4bn a year, BMA estimates
BMA judicial review over cost of government’s pension mistakes is dismissed
NHS weight loss programme produces moderate benefit, analysis shows
Ethnic minorities receive markedly worse healthcare in every US state, finds Commonwealth Fund
Helen Salisbury: Sick notes and a national illness service
NHS England looks to cut back on doctors’ statutory and mandatory training
Why I . . . practise Brazilian jiujitsu
Latest articles
News

Europe is seeing “devastating” rise in health harms from extreme weather events, experts warn
US pregnant workers get new legal protections, but not paid time off
African countries recall batch of Johnson and Johnson cough syrup because of toxicity concerns
Teesside trust is fined £200 000 over failures in care of two patients who died by suicide
US Supreme Court allows Idaho to ban gender affirming care for minors—for now
Sixty seconds on . . . smoking trends
Sunak is accused of “harmful” rhetoric amid plans to remove sick note responsibility from GPs
Doctors protest outside GMC offices to demand climate action
Research
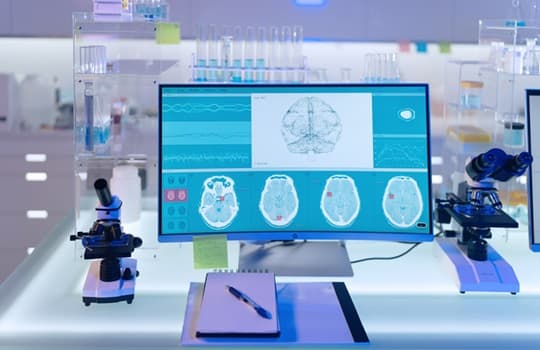
TRIPOD+AI statement: updated guidance for reporting clinical prediction models that use regression or machine learning methods
Impact of large scale, multicomponent intervention to reduce proton pump inhibitor overuse
Esketamine after childbirth for mothers with prenatal depression
Glucagon-like peptide 1 receptor agonist use and risk of thyroid cancer
Quantifying possible bias in clinical and epidemiological studies with quantitative bias analysis: common approaches and limitations
Use of progestogens and the risk of intracranial meningioma
Delirium and incident dementia in hospital patients
Comment
A new approach to oral health can lead to healthier societies
When will Canada have national pharmacare?
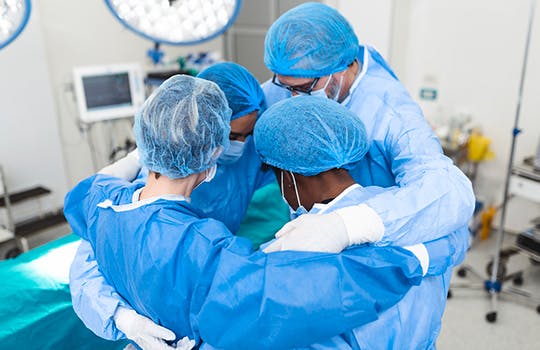
Healthcare professionals deserve support services tailored to their needs
Doctors should not be simply the ghost in the machine
Why hospital capacity is more complex than bed capacity
Partha Kar: We need to level up all staff, not level down doctors
Mental health support for doctors—a vital yet fragile lifeline
Breaking free from the stigma of diabetes
Helen Salisbury: With the NHS in crisis, why is Labour looking to private hospitals as the solution?
Health literacy matters
Education
How to communicate about climate change with patients
Alternative routes into clinical research: a guide for early career doctors
Advances in management of heart failure
Non-acute heart failure management in primary care
Group A beta-haemolytic streptococcal infection in children
Secondary prevention of cardiovascular disease, including cholesterol targets: summary of updated NICE guidance
Effectiveness and safety of drugs for obesity
Dry eye disease management
Caring is the invisible piece of the stroke recovery puzzle
Stroke rehabilitation in adults: summary of updated NICE guidance
Workforce
BMJ Medicine
Identification of patients undergoing chronic kidney replacement therapy in primary and secondary care data
Apr 18
New insights into understanding obesity
Mar 29
Characterization of approval status, endpoints, results, and recommendations for oncology drug treatments from the NCCN
Apr 5
Practical implications of the ADNEX risk prediction model for diagnosis of ovarian cancer
Apr 3
UK Jobs
Current issue
Most read
1.
Effect of exercise for depression: systematic review and network meta-analysis of randomised controlled trials
2.
Ultra-processed food exposure and adverse health outcomes: umbrella review of epidemiological meta-analyses
3.
Use of progestogens and the risk of intracranial meningioma: national case-control study
4.
Multiple adverse outcomes associated with antipsychotic use in people with dementia: population based matched cohort study
5.
Advances in management of heart failure
6.